Clinical Science | Surgical Oncology
ASSOCIATION OF BRAFV600E MUTATION AND THE AGGRESSIVE BEHAVIOR OF PAPILLARY THYROID MICROCARCINOMA: A META-ANALYSIS OF 29 STUDIES
M Aboueisha, A Attia, A Elnahla, A Farhoud, M Youssef, M Hussein, M Shama, J Russell, E Toraih, R Tufano, E kandil
ePoster Presenter: Mohamed Aboueisha MD, Tulane School of Medicine
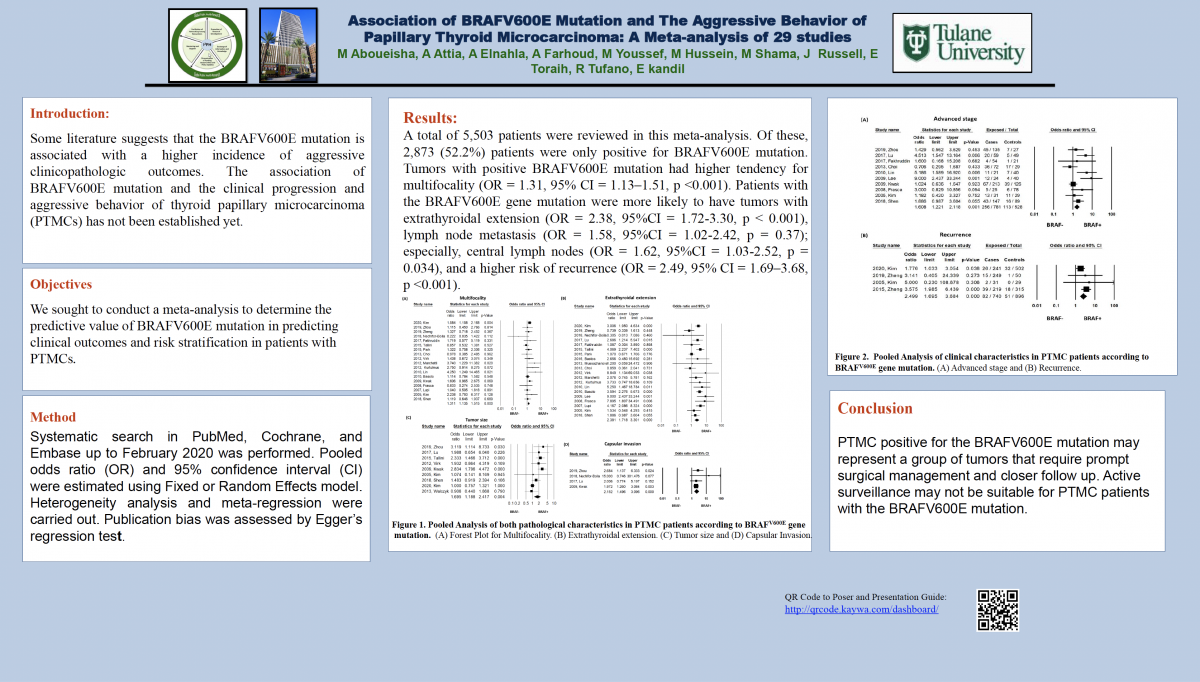
Background: Some literature suggests that the BRAFV600E mutation is associated with a higher incidence of aggressive clinicopathologic outcomes. The association of BRAFV600E mutation and the clinical progression and aggressive behavior of thyroid papillary microcarcinoma (PTMCs) has not been established yet.
Objectives: We sought to conduct a meta-analysis to determine the predictive value of BRAFV600E mutation in predicting clinical outcomes and risk stratification in patients with PTMCs.
Methods: Systematic search in PubMed, Cochrane, and Embase up to February 2020 was performed. Pooled odds ratio (OR) and 95% confidence interval (CI) were estimated using Fixed or Random Effects model. Heterogeneity analysis and meta-regression were carried out. Publication bias was assessed by Egger’s regression test.
Results: A total of 5,503 patients were reviewed in this meta-analysis. Of these, 2,873 (52.2%) patients were only positive for BRAFV600E mutation. Tumors with positive BRAFV600E mutation had higher tendency for multifocality (OR = 1.31, 95% CI = 1.13–1.51, p <0.001). Patients with the BRAFV600E gene mutation were more likely to have tumors with extrathyroidal extension (OR = 2.38, 95%CI = 1.72-3.30, p < 0.001), lymph node metastasis (OR = 1.58, 95%CI = 1.02-2.42, p = 0.37); especially, central lymph nodes (OR = 1.62, 95%CI = 1.03-2.52, p = 0.034), and a higher risk of recurrence (OR = 2.49, 95% CI = 1.69–3.68, p <0.001).
Conclusion: PTMC positive for the BRAFV600E mutation may represent a group of tumors that require prompt surgical management and closer follow up. Active surveillance may not be suitable for PTMC patients with the BRAFV600E mutation.